Osteoarthritis
Osteoarthritis is the most common disease of the joints, and one of the most widespread of all chronic diseases.
Frequently described as ‘wear and tear’, its prevalence increases steadily with age and by retirement age the associated radiological changes can be observed in over half the population.
Symptoms can vary from minimal to severe pain and stiffness, but overall the disease is responsible for considerably reduced wellness and is a common reason for GP consultation.
What is osteoarthritis?
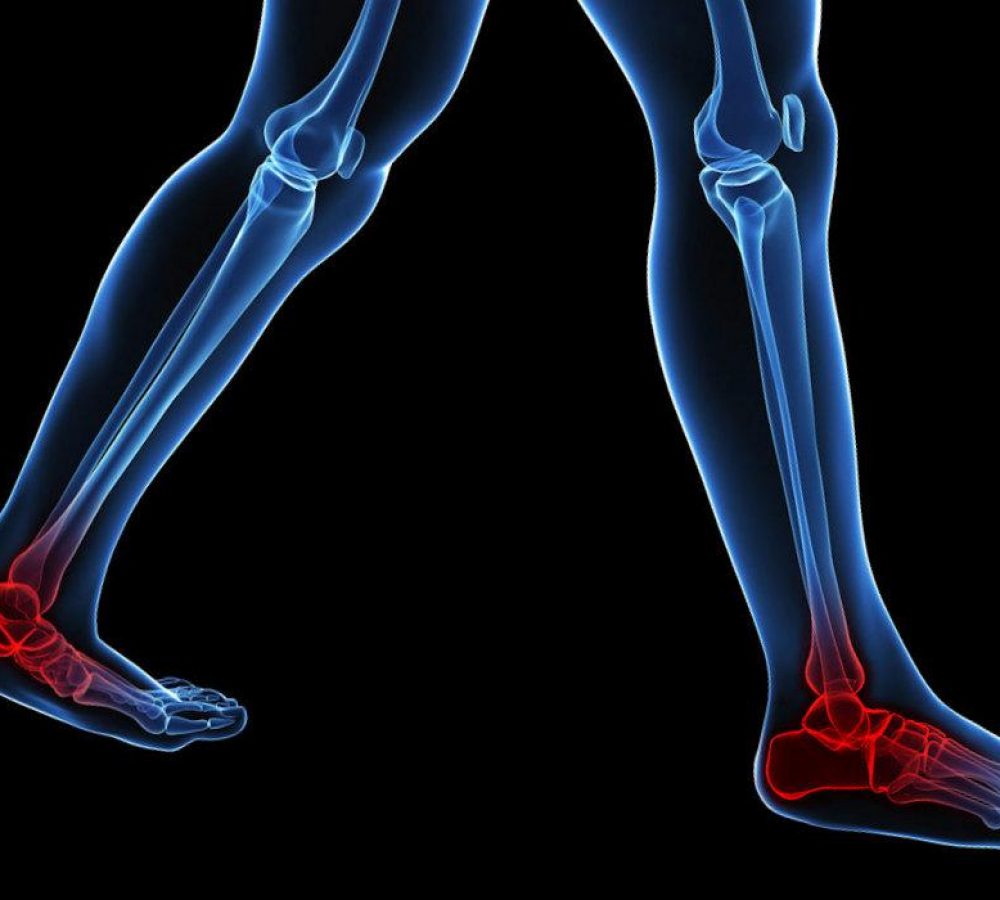
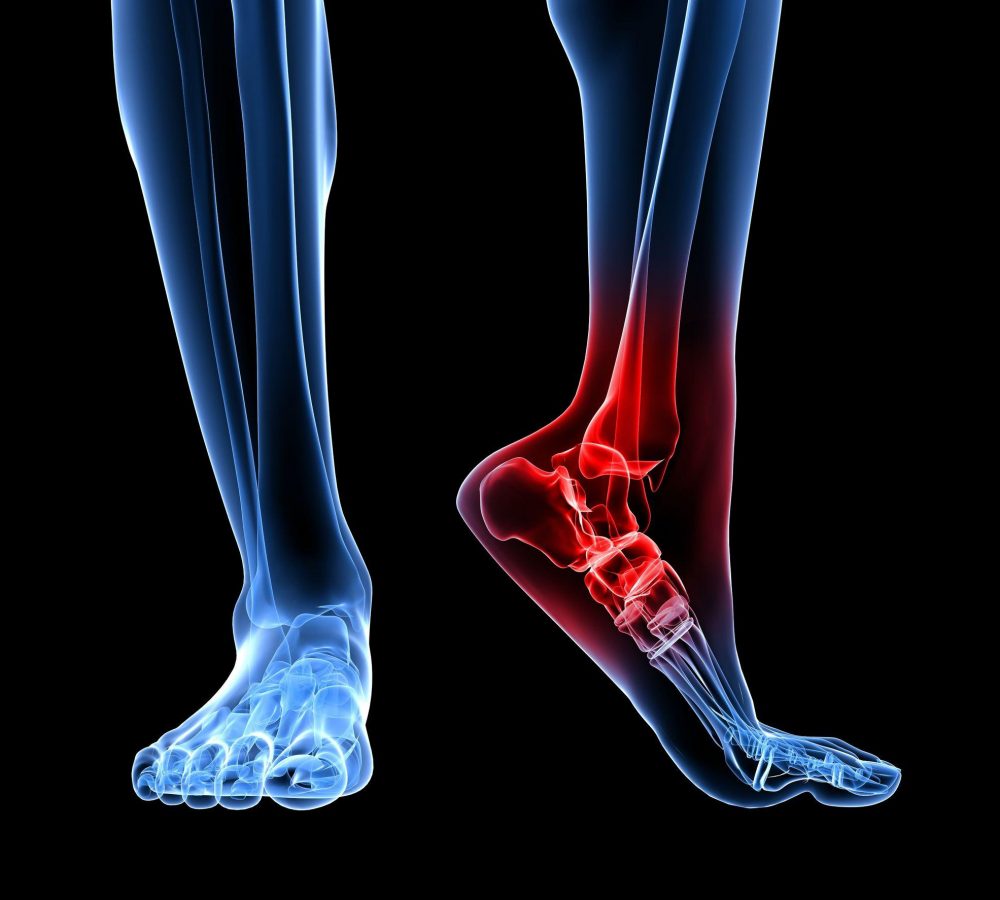
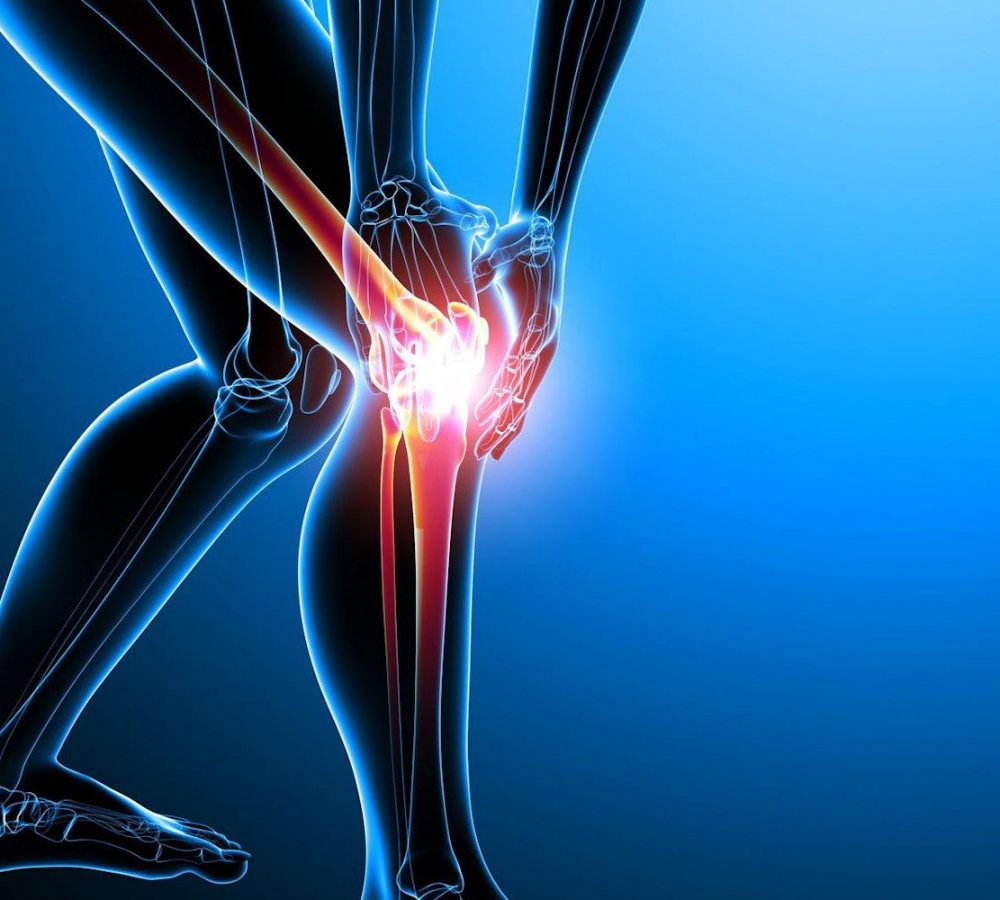
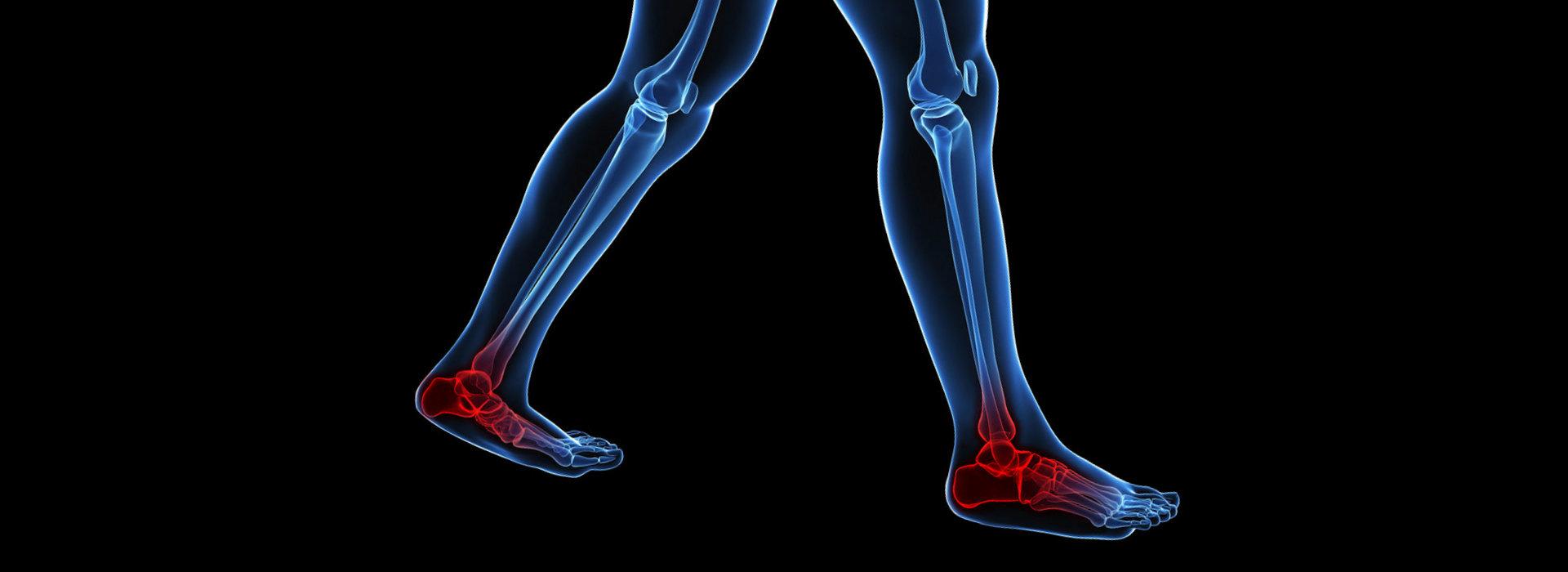
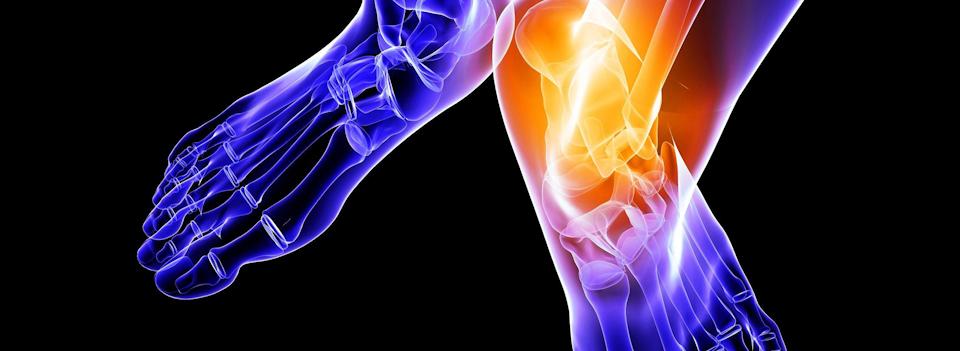
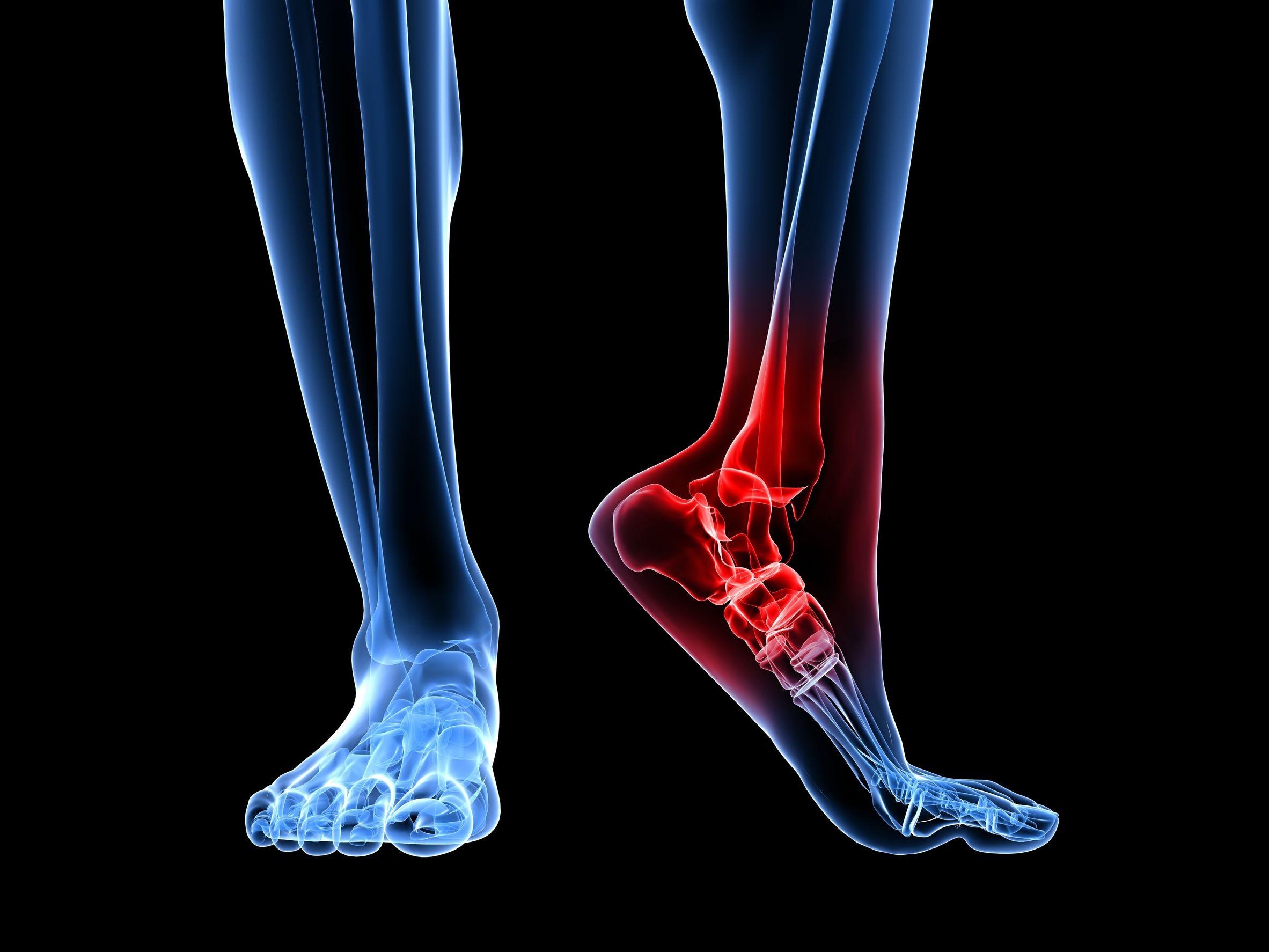
Osteoarthritis (OA) refers to a clinical syndrome of joint pain accompanied by varying degrees of functional limitation and reduced quality of life. It is by far the most common form of arthritis and one of the leading causes of pain and disability worldwide. Any synovial joint can develop osteoarthritis but knees, hips and small hand joints are the peripheral sites most commonly affected. In the foot the ankle has the most prevalence of OA followed by the big toe joint.
Theory
Osteoarthritis is a metabolically active, dynamic process that involves all joint tissues (cartilage, bone, synovium/capsule, ligaments and muscle). Key pathological changes include localised loss of articular (hyaline) cartilage and remodeling of adjacent bone with new bone formation (osteophyte) at the joint margins. This combination of tissue loss and new tissue synthesis supports the view of osteoarthritis as the repair process of synovial joints. A variety of joint traumas may trigger the need to repair, but once initiated all the joint tissues take part, showing increased cell activity and new tissue production. In general, osteoarthritis is a slow but efficient repair process that often compensates for the initial trauma, resulting in a structurally altered but symptom-free joint. In some people, however, either because of overwhelming insult or compromised repair potential, the osteoarthritis process cannot compensate, resulting in continuing tissue damage and eventual presentation with symptomatic osteoarthritis or ‘joint failure’. This explains the extreme variability in clinical presentation and outcome, both between individuals and at different joint sites. The specific targeting of osteoarthritis for certain joints remains unexplained, but one hypothesis suggests an evolutionary fault where joints that have most recently altered are biomechanically under designed and thus more often fail.
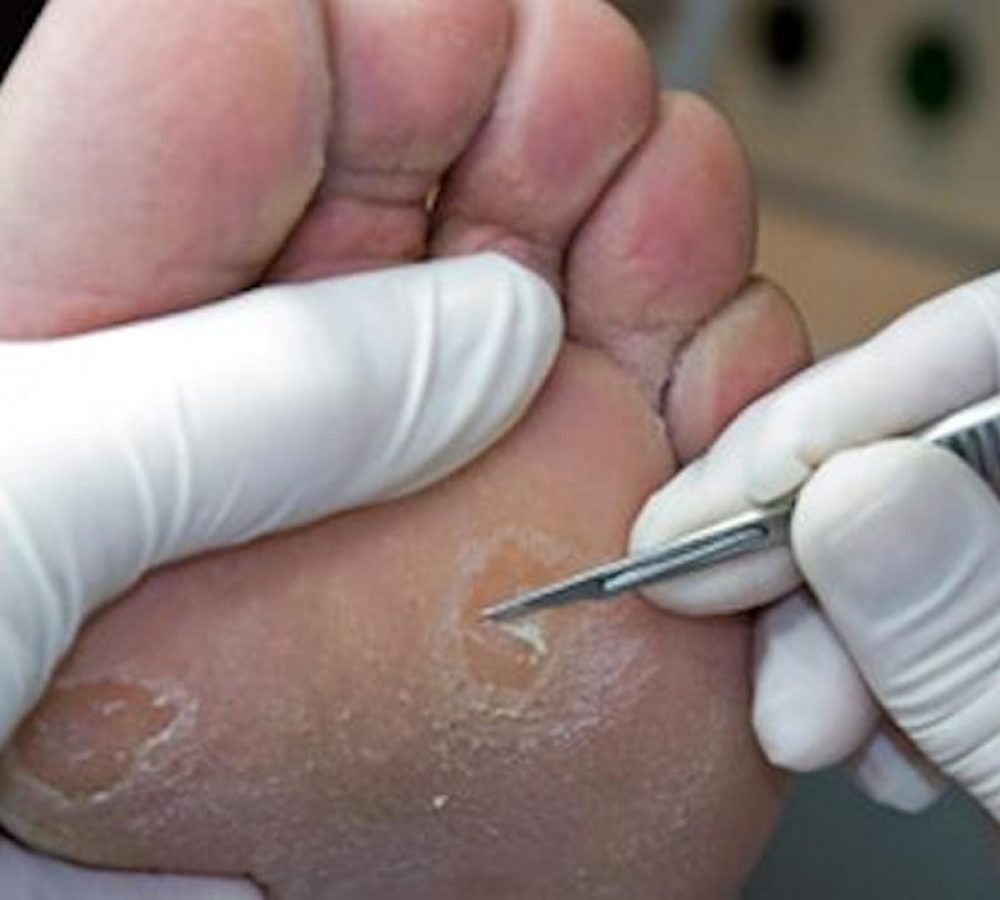
Treatment of osteoarthritis
At THE foot mechanic, treatment options include; education, advice and access to strengthening/stretching exercises, footwear, supports and braces, bio-mechanical assessment, orthotic prescription, acupuncture, manual therapy and referral to your GP to request surgery as a last resort if needed.